PRESCRIPTION: HD

A daily selection of features, industry news, and analysis for tech managers. Sign up below.
You are now subscribed
Your newsletter sign-up was successful
Telemedicine Deployment Increases Efficiency for Ontario’s Appletree Medical Group
Patients who walk into one of Appletree Medical Group’s private clinics in Toronto and Ottawa, Ontario, Canada have a choice. They can either sit down and wait an hour or more to see a live, in-person doctor. Or they can cut their wait by being treated by a two-way telemedicine link.
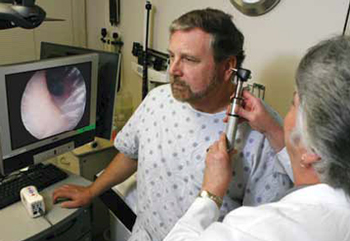
Using telemedicine, E.R. doctors in remote locations can get access to top-flight specialists quickly and easily.If the patient chooses the telemedicine option, they are taken to a room equipped with a videoconferencing camera, monitor, and microphone. The patient is then connected with a telemedicine assistant (TA). The TA—typically a nurse or doctor in residence—remotely records the patient’s medical history on an electronic medical record (EMR). Physical symptoms like rashes or bruises are capture with a high-resolution camera. There’s also an electronic stethoscope that lets the TA hear the patient’s heart beat and breathing. Blood pressure can also be taken and transmitted, and other tests ordered.
When all this data has been recorded, the patient is referred to a doctor for the telemedicine diagnosis. Once the consultation is over, the doctor can prescribe medicine, with the prescription being printed electronically at the local Appletree clinic. The patient can also be sent for further tests, or referred to a local hospital, all without actually seeing the doctor in person.
The Appletree trial is being facilitated by the Ontario Telemedicine Network (OTN). OTN is a non-profit organization funded by the Ontario government, for one very simple reason: The province’s health expenses are skyrocketing, and the cash-strapped government is looking for cost-effective alternatives to traditional medical care. (In Ontario, doctors and medical facilities are paid for by the Ontario government.)
According to OTN CEO Dr. Ed Brown, telemedicine is also making a difference to the province’s bottom line. “In 2011, we avoided expenditures of about $45 million in Northern Ontario alone, by treating patients through telemedicine who otherwise would have been transported a total of 60 million miles for treatment,” Dr. Brown tells AV Technology Magazine. “That’s just the tip of the iceberg. Once telemedicine is a province-wide reality, we could save Ontario taxpayers many more millions of dollars, while improving the health care they receive.”
A Geographical Conundrum
A daily selection of features, industry news, and analysis for tech managers. Sign up below.
Geography is a driving force behind OTN. Ontario is a huge province that covers some 400,000 square miles. To put this in context, it’s the size of Texas and California combined.
To make matters worse, 12 million Ontarians live close to the U.S. border in the south. The remaining one million are scattered across the province—often in rural and remote communities too small to support specialized medical care. To take the Texas/California analogy further, it is as if 12 million potential patients live in the Los Angeles area, with the remaining one million scattered throughout the rest of the combined states.
This is why telemedicine has been embraced by the Ontario government. And its acceptance is growing: In 2011/12, OTN delivered care to more than 204,000 patients and expects that to grow another 50 percent this year.
A Telemedicine Backbone, Standards-Setter, and Matchmaker
In a far-flung territory like Ontario, telemedicine makes sense—but only if it is deployed in a consistent, interoperable and standards-based manner.
This is where the Ontario Telemedicine Network comes in. As one of the largest telemedicine systems in the world, it manages the de facto network that links together its membership.
OTN’s membership is huge: “We have 1500 members, including every hospital in the province,” said Dr. Brown. “We have about 125 primary care sites, 350 mental health agencies, 94 long-term care facilities, and many of the medical and nursing schools.”
Besides managing Ontario’s telemedicine network—and acting as traffic cop to keep things running smoothly—OTN sets equipment standards for its users.
“We have standardized on Cisco/Tandberg, Polycom, and Vidyo videoconferencing technology, and are open to our members’ choices so long as their equipment is compatible and meets network standards,” Dr. Brown said. “The level of sophistication of the equipment they use is up to them. Some only want basic two-way videoconferencing. Others want a full range of diagnostic tools to send and receive data over long distances.”
Finally, OTN helps its rural and remote members connect to the medical specialists they are looking for. “It can be difficult for small community health centers to know where to find the experts they need,” said Dr. Brown. “So we do our best to connect them with the right specialists: In the telemedicine arena, we’re not just a network provider and standard-setter, we’re a matchmaker.”
A Range of Services
OTN’s bread-and-butter is videoconferencing. But these two-way links are not just used for telemedicine: The organization also supports distance education for medical professionals— ‘Participate in Rounds and other accredited continuing health education at every hospital and hundreds of other sites across Ontario,’ said OTN. ca—and cost-effective virtual meetings: ‘Avoid travel expenses and reduce your carbon footprint’. “We also support webcasts and webconferences,” said Dr. Brown. “We pretty much do it all.”
On the practical medical side, OTN is breaking new ground with telehomecare. “There are many instances where patients with chronic disease can be treated at home, where they are more comfortable and it costs less to take care of them,” Dr. Brown said. “We can pair these patients with nurses who act as their coaches. The patient’s home is equipped with equipment that connects over a secure VPN. After being trained by a nurse, they can take and transmit their own vital readings. This data is monitored by their assigned Family Health Team, ensuring that any issues are dealt with promptly.”
To prove the validity of telehomecare, OTN recently tested at-home treatment of more than 800 patients with Congestive Heart Failure or Chronic Obstructive Pulmonary Disorder. The results were impressive: Among the group being treated using Telehomecare, there was a 65 percent reduction in the average number of hospital admissions; a 72 percent cut in the average number of Emergency Room visits; and a staggering 95 percent reduction in the average number of walk-in clinic visits. Based on these results, OTN is currently planning a much broader roll out of the program.
“In the telemedicine arena,” OTN CEO Dr. Ed Brown says, “we’re not just a network provider and standard-setter, we’re a matchmaker.”OTN has also launched an Emergency Services Program. This program supports Emergency Rooms in smaller hospitals, where there may not be physician expertise available to support complex emergency care—such as acute stroke, burns, or multiple trauma. Using telemedicine, E.R. doctors in these locations can get access to top-flight specialists quickly and easily. This enables improved patient care and potentially fewer patient transfers to larger urban hospitals.
All of these services are based on a realtime model. But mindful that not every medical situation is time-sensitive, OTN also offers a ‘Store Forward’ application of telemedicine. Currently used in dermatology, Otn.teledermSF. lets a nurse or doctor digitally photograph a skin condition, and then upload the photo and relevant patient data to a secure server. “An Ontariobased dermatologist accesses the server to review the information, returning a diagnosis and suggested treatment to the referrer,” said OTN.ca, “all without a long wait, added costs or travel time for patients.”
Return on Investment
Telemedicine will not replace every kind of in-person medical assessment. But it may improve wait times for patients while reducing the costs and time associated with traveling for care. Meanwhile, for those one million Ontarians not living along the Canada-U.S. border, telemedicine could radically improve the quality of health care they currently receive—and eliminate the need for costly, timewasting travel.
So how much could telemedicine save Ontario taxpayers? Well, $48.7 billion has been allocated for healthcare system in 2012-2013. That is over 38 percent of the province’s total budget. Given that Ontario is trying to cut its current $15.3 billion budget deficit, anything that can reduce the amount spent on health care while maintaining the quality of care is a welcome option.
James Careless is an Ottawa-based writer who covers audio and video developments, as well as the business of technology. Reach him at jamesc@tjtdesign.com.
INFO
Ontario Telemedicine Network (OTN)
otn.ca
Key Elements for the End User/ / /
ROI:
“It is difficult to put a figure on it, but we think that telemedicine could eventually account for 25 percent of all patient/health care provider consultations. That’s just our estimate; some sources believe the number could be as high as 40 percent. But either way, telemedicine is becoming a reality in Ontario—improving patient care while reducing cost pressures and wait times in the process.” —OTN CEO Dr. Ed Brown
James Careless is an award-winning freelance journalist with extensive experience in audio-visual equipment, AV system design, and AV integration. His credits include numerous articles for Systems Contractor News, AV Technology, Radio World, and TV Tech, among others. Careless comes from a broadcasting background, with credits at CBC Radio, NPR, and NBC News. He currently co-produces/co-hosts the CDR Radio podcast, which covers the Canadian defense industry. Careless is a two-time winner of the PBI Media Award for Excellence.

