Government Penalties on Hospitals Can Mean Business for AV Integrators

A daily selection of features, industry news, and analysis for AV/IT professionals. Sign up below.
You are now subscribed
Your newsletter sign-up was successful
What do Massachusetts General Hospital, Barnes-Jewish Hospital in St. Louis, and University of Michigan Hospital all have in common? They are included on a list of 2217 hospitals across the country that will be penalized for readmitting too many Medicare patients within 30 days of release. So how is this an opportunity for you? Let’s take a look.
It is estimated that the re-hospitalization of nearly one in five Medicare patients within 30 days of being discharged is costing the government $17 billion per year. Researchers believe that the root cause is the process known as “post-acute care transition,” which is the process by which a patient typically moves from the hospital to home. The federal government believes that many of these are avoidable and under the Patient Protection and Affordable Care Act (a.k.a. Obamacare) have begun imposing financial penalties on hospitals deemed to have too many readmissions of heart failure, heart attack, and pneumonia patients.
Phase one of the program began October 1, 2012 with 307 of the 2217 hospitals receiving the maximum allowable penalty of 1 percent of their regular Medicare reimbursements. Over the next three years the issue will continue to grow as the penalty increases, reaching 3 percent of reimbursement in October 2015. Although the penalties are applied only to Medicare patients, private insurers will often follow the payment guidelines of Medicare, increasing the focus on this issue by hospitals.
Article continues belowAs you would imagine, the penalties are not very popular with hospitals, and they are aggressively looking for new ways of doing business to improve the patient transition process. Most of their attention is focused around three core areas — patient support, improving self-management capabilities, and increasing accessibility to needed information and tools. All of these areas provide new opportunities for aligning multiple technologies that our industry already provides and the possibility to expand into some new product categories.
At the top of the list is visual communications. Many of us already have experience with video communications technology in telehealth, but most of the applications have been based within or between hospitals. These applications typically include telestroke programs, remote surgical consultation, remote specialist consult, ER interpreter services, and training and education for residents/interns and hospital staff.
Advancements in today’s technology allows for the extension of visual communications to almost anywhere via smartphones, tablets, and client-based applications for PC. This technology has not only become further reaching, but also simpler to use and more cost-effective. The ability to communicate and access a patient remotely, as well as on a more frequent basis, offers great potential for improvement in the patient transition process. Additionally, these same devices can be used by patients to access video-based educational information.
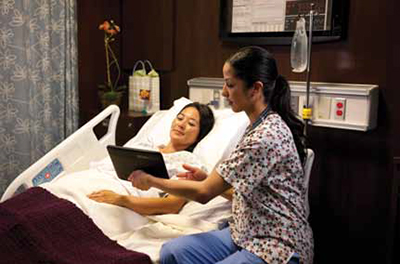
Another area of expertise in the AV industry is environmental monitoring and control. The ability to monitor environment conditions, including temperature and carbon monoxide, are typical in today’s home automation system. Transitioning these skills to in-home healthcare monitoring applications isn’t that big of a leap. Proximity smart sensors and some backend analytics and it quickly becomes easy to identify a patient’s routine changes at home. Combining this with a variety of readily available telehealth smart devices ranging from pulse monitors to weight scales, and the possibilities become endless.
A daily selection of the top stories for AV integrators, resellers and consultants. Sign up below.
The opportunity created by the imposed penalties of the Affordable Care Act opens the door for new applications, but with this opportunity comes a set of unique challenges. Over the years, we have seen slow adoption of telemedicine technologies, primarily due to concerns around return on investment from the healthcare industry. Being in the technology field, we are very comfortable with the next generation of technology being introduced in shorter and shorter timeframes, but hospital administrators are looking for technology investments with more stability.
The bottom line is “listen and learn” from your client. The measurement in this scenario is reducing the Medicare penalties by reducing the quantity of patients readmitted within the 30-day timeframe. Constantly measure the cost of your solution against what process improvement and efficiencies it will create, and you will be successful.
R. Randal Riebe (randy.riebe@polycom.com) is the director of AV integrator business development at Polycom.
